Imaging and Treatment of Cancer through Combinations of Nanoparticles and Hormones
Carola Leuschner, Ph.D.
This article was adapted from a lecture given by Professor Carola Leuschner, Ph.D. during Terasem Movement, Inc.’s 3rd Annual Workshop Webinar on Geoethical Nanotechnology, July 20th, 2007.
Dr. Leuschner discusses in detail, the work of her research team at the Pennington Biomedical Research Center, Baton Rouge Campus of the Louisiana State University, which employs nanotechnology aimed at targeting and eradicating breast cancer cells while leaving normal cells unaffected.
I will give a brief background about nanotechnology, cancer, targeting cancer, and then talk about preclinical development of a contrast agent for magnetic resonance imaging (MRI) [1], which includes synthesis, studies in vitro and in vivo [2] testing; magnetic resonance imaging; and then preclinical development of a new treatment for cancer, specifically in metastatic disease. Again, synthesis and in vitro and in vivo testing are involved.
Nanotechnology involves particles that are between one and  two hundred nanometers. To have a comparison, about a million nanometers is the size of a dust mite, so you can imagine how small nanoparticles are.
two hundred nanometers. To have a comparison, about a million nanometers is the size of a dust mite, so you can imagine how small nanoparticles are.
The small size has many advantages because nanoparticles are smaller than cells, and smaller than a subpopulation of cells, the so-called organelles in cells. Therefore, nanoparticles can be used to infiltrate sub cellular compartments.
They are too small to obey classical physics, however, too large to apply to quantum physics. They have a large surface, and due their small size and modification change properties are certainly abundant. They are small enough to enter tumor cells and also normal cells, and they can be used for biomedical applications.
Applications in nanotechnology and medicine would be, for example: building sensors for biomolecules. It can be used for imaging, for example, if the contrast agent is linked to a delivery system. They are for treatments through hyperthermia, and also for building biomedical devices.
Cancer as a disease is still untreatable. If you look at development and changes in death rates in the U.S., heart disease death rates between 1950 and 2001 definitely dropped way down.
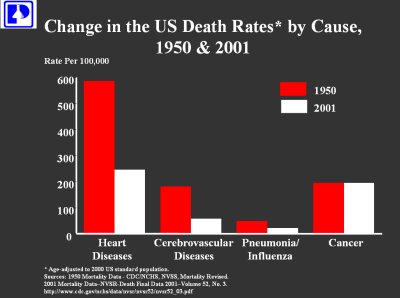
Image 1
However, cancer death rates still stay stagnant, and there was no improvement in cancer treatments regarding survival. The main reason for that is that there is something which is called metastatic disease [3]. We have primary tumors and metastatic disease to distinguish.
Primary tumors can be treated if early recognized and diagnosed; if the patient contracts metastatic disease (a disease from the primary tumor building up metastases in  lymph nodes, bone marrow, and other parts of the the body), that stage of the disease is causing the five year survival rate to drop drastically in lung cancer, and less than 10 percent and 20 percent in colorectal cancer. Therefore, we have less than 50 percent survival rate in patients with metastatic disease.
lymph nodes, bone marrow, and other parts of the the body), that stage of the disease is causing the five year survival rate to drop drastically in lung cancer, and less than 10 percent and 20 percent in colorectal cancer. Therefore, we have less than 50 percent survival rate in patients with metastatic disease.
The big problem in that case is also metastatic disease is not readily detectable. Nanotechnology can certainly build a bridge in the gap to detect early stage metastatic
disease. Nanoparticles can be designed for implant and hormone treatment modalities to increase treatment efficacy.
Currently applied methods for detecting metastatic disease, we can distinguish between invasive methods, which require anesthesia and, for example, among those are tissue biopsies; the tumor needs to be at least greater than one centimeter in diameter; bone marrow aspiration is very invasive and it is also painful.
In the case of noninvasive methods for example mammography or ultrasound, the tumor needs to be about one centimeter and has a 36 percent detection rate by ultrasound. More sensitive methods of detection are X-ray, PET and CT [4], that can detect 60 percent of the lesions which are already missed in a mammogram, and they offer higher sensitivity, and can detect tumor sizes between 6 millimeter and one centimeter.
Magnetic resonance imaging (MRI) can certainly be improved dramatically by using a contrast agent. Looking at contrast the agents, I will further elaborate on that method to develop better agents. There are already clinically approved contrast agents for MRI on the market. They accumulate mainly in the liver and, therefore, can certainly improve the resolution for magnetic resonance imaging in this organ. Another contrast agent is the iron oxide nanoparticle of 25 nm size, for example, that would be applicable for the detection of lymph node metastases.
Both of these magnetic resonance imaging contrast agents have the disadvantage that they do not necessarily accumulate within the cancer cells. We want to specifically detect the cancer cells, not the surrounding tissue, and also reduce the background to have a higher sensitivity.
Here, the next graphic shows nanoparticles for detection of lymph node metastases in prostate cancer patients. These nanoparticles are carried into the lymphnodes by lymphocytes, and you get basically an indirect image by having the surrounding of the tumor itself labeled.
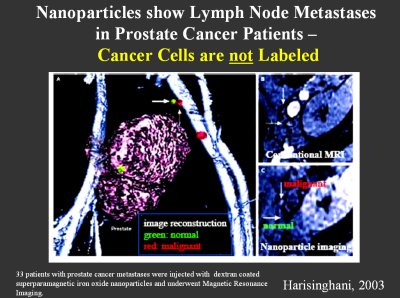
Image 2 [Click above for larger image]
Whatever area is not occupied by the tumor cells in the lymph node, as found in that approach, is taken up by the lymphocyte containing nanoparticles. You have a differential image acquisition; it is an indirect acquisition. You have to make two magnetic resonance images (at least two), to get a contrast image in order to make a diagnosis.
In our approach, we seek to directly label cancer cells in vivo. In order to do that we
have been looking at surface receptor expressions of cancer cells and we have found
(others have also published) that hormone receptors, luteinizing [5] hormone-releasing
hormone receptors, are over-expressed in most of the ten leading cancer cases. For example, prostate cancer, colon cancer, even melanoma and cancer of the kidney, breast cancer, etc.
Footnotes
1. Magnetic Resonance Imaging (MRI) – n. The use of a nuclear magnetic resonance spectrometer to produce electronic images of specific atoms and molecular structures in solids, especially human cells, tissues, and organs.
The American Heritage STEDMAN’S Medical Dictionary. Boston, New York: Houghton Mifflin Company, 2004: 480.
2. In vitro – adj. In an artificial environment outside a living organism. In vivo – adj. Within a living organism.
The American Heritage STEDMAN’S Medical Dictionary. Boston, New York: Houghton Mifflin Company, 2004: 424.
3. Metastatic – adj. 1. Transmission of pathogenic microorganisms or cancerous cells from an original site to one or more sites elsewhere in the body, usually by way of the blood vessels or lymphatics. 2. A secondary cancerous growth formed by transmission of cancerous cells from a primary growth located elsewhere in the body.
The American Heritage STEDMAN’S Medical Dictionary. Boston, New York: Houghton Mifflin Company, 2004: 506.
4. PET - Positron emission tomography - a nuclear medicine medical imaging technique which produces a three-dimensional image or map of functional processes in the body.
http://en.wikipedia.org/wiki/Positron_emission_tomography January 2, 2008 4:43PM EST
5. Luteinizing - v. lu·te·in·ized, lu·te·in·iz·ing, lu·te·in·iz·es - v.tr. To cause the production of a corpus luteum in. v.intr. To develop into or become part of the corpus luteum.
http://www.thefreedictionary.com/luteinize January 2, 2008 4:51PM EST
1 2 3 4 Next Page>